All the way, my Savior leads me;
What have I to ask beside?
Can I doubt His tender mercy,
Who through life has been my guide?
Heav’nly peace, divinest comfort,
Here by faith in Him to dwell!
For I know, whate’er befall me,
Jesus doeth all things well.
We had our fourth ultrasound on Thursday, and the phrase ‘tender mercy’ from the first verse of “All the Way My Savior Leads Me” was echoing through my mind during the scan and has been ever since. We sense God’s mercies so keenly and know that He is leading us through this experience. What a joy to fulfill this assignment He has given us knowing that HE “cheers each winding path [we] tread; Gives [us] grace for every trial; Feeds [us] with the living bread!” He truly is sustaining us in every way.
Our third ultrasound (8 weeks ago) was rather unremarkable in that we learned a bit more about baby’s condition but it wasn’t ‘game-changing.’ Baby’s bladder was almost the size of an adult’s bladder at that point, and it was acting as a flotation device, preventing him from turning or flipping. Baby Joel could wiggle and twist and move his arms and legs, but he was expected to stay in his transverse position, with his head/face snuggled into my right hip area. We noted on this scan that his hands were not contracted as some T-13 babies’ are, and he appeared to have a normal number of fingers. The only obvious external deformity was a clubbed right foot, which is very common to trisomy kids. He appeared to not be ‘hydroptic’ at this point, so the concerns for my blood pressure were down-graded, taking a lot of pressure off me to be constantly monitoring it – pun intended!
It was after U/S three that the reality of the long-term nature of this pregnancy began to settle in. I remember vividly a dark, late night when I felt quite trapped and overwhelmed at the realization that I would most likely carry Joel to a full 40 weeks. This is not to say that I was hoping he would be born early. I didn’t really want that either. How can one even begin to know what a ‘best case scenario’ or ‘worst case scenario’ is in a situation like this? Of course nobody knows when he will be born, and the constant awareness that I need to be ready to deliver him within two days of his passing, whenever that may be, can be emotionally tiring. But when the perinatologist explained that he is doing quite well, in spite of his anomalies, because he is hooked up to me – a perfect life-support system – and that his anomalies most likely won’t be overwhelming to him until he needs to do life on his own, I knew I needed to mentally prepare for the long-term while staying ready for any possible time-frame.
Ultrasound four on 11/19 felt much more important, as it was now time to start discussing Joel’s condition in relationship to how he will be delivered and also to begin to make predictions for what his condition will be if he is born alive. We received several tender mercies from God in connection with this ultrasound.
First, Jeff decided to go along, and a rainy day made it all the easier for him to get away from work for a few hours. This is the first he’s been able to join me since U/S one, and the timing couldn’t have been more perfect, as the discussions with Dr. B were so important. It was a comfort to be together to establish common expectations for Joel’s delivery and care after birth.
The perinatologist met with us prior to the scan and then was with us for the entire ultrasound, even doing part of it himself! I can’t being to say enough about the amazing and wonderful medical professionals we have met on this journey. To relate to a doctor who is personable and supportive but not overly sympathetic or emotional, who is incredibly smart and completely knowledgeable, and who is unrushed in examining our baby and discussing our care is truly a great gift and the second of the tender mercies we experienced that day!
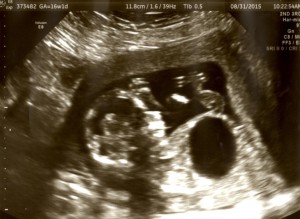
A week ago, I sensed that Joel had changed positions in spite of his bladder size, based on where I was feeling his kicks, and the U/S proved this to be correct. His new frank-breech position allowed for a third tender mercy: we finally got a close look at his adorable face! Aside from the technical aspects of his delivery and overall condition, I really wanted to satisfy a personal curiosity that hadn’t yet been answered. Does he have any of the severe facial deformities common to T-13 babies? I was secretly hoping for a 3-D view of his face, if/when they were able to scan it, and without my asking, the tech immediately switched to the highest possible resolution for the scan when she got to his face. While I was prepared to love him no matter the condition of any part of him, I knew from googling ‘Trisomy 13’ a hundred times that his face might be quite difficult to view if he had no eyes and/or a bilateral cleft lip/palate, etc. I was especially concerned about how I would prep our other kids for this reality. It was a true joy – and a third mercy – to see that he does not have significant facial issues. In fact, Jeff and I both thought immediately that he looks a lot like Lydia. It was fun to bond with him in a new way through seeing his tiny features and even a little smile at times.
Joel does have one significant outward reminder of how unwell he is internally. His right leg ends at the knee, and the clubbed foot at its end looks a lot like Nick Vujcic’s (http://www.lifewithoutlimbs.org). Jeff calls it his little ‘duck foot,’ and somehow even that looks cute to us at this point on our journey.
The largest amount of scanning time was spent on Joel’s heart. He has an Atrial Septal Defect (ASD), and one of the chambers of his heart is significantly smaller than normal. Issues remain with his bladder, kidneys, brain, and overall growth. At the end of the scan, we asked which of his many defects will be the most problematic for him after birth, and Dr. B was quick to say that it would be his heart. Because of the ASD, he will probably live for only a few hours or possibly days, if he survives birth.
How he will be born will depend on many factors which can’t be known until the time comes. This continues to be a matter for prayer. I would very much like to avoid a C-section, but since this delivery would be a VBAC, the timing of labor and the requirements for his positioning and physical condition will all have to align perfectly for this to occur. I know God is able to make it happen, but I’m also trying to stay mentally prepared for any possibility in this area too.
Today marks the beginning of the third trimester! We truly look forward to meeting Joel and holding him in our arms, though our hearts break at the thought of surrendering Him back to God after such a short time together. Only 12 weeks or fewer left with our precious baby boy.